Debunking myths of urinary symptoms and prostate cancer
Time to 'rebrand' most prostate cancer as aymptomatic
By Howard Wolinsky
Messaging in the popular media and even in medical guidelines is sending exactly the wrong message about an association between urinary symptoms and curable prostate cancers.
In reality, there is virtually no relationship between most prostate cancers and symptoms, such as frequent or painful urination.
Professor Vincent J. Gnanapragasam, of the University of Cambridge, and colleagues stress in an article in the current BMC Medicine that these misconceptions “may be preventing earlier presentation and better survival outcomes” with prostate cancer.
The researchers say the public doesn’t generally understand that these urinary symptoms are not symptoms especially for “curable prostate cancer.“
Gnanapragasam told me the “curable” group “includes anyone who does not die of prostate cancer whether that be because of radical treatment or is on surveillance and never needs treatment—indeed, any cancer that gains from being found early such that a man does not die of the prostate cancer Once it’s metastatic or very local advanced that chance is not there.”
The researchers say that patients who wait for symptoms to be screened to see their general practitioners may be missing early diagnosis and management.
Also, the researchers said there is a need to “rebrand” curable prostate cancers as an asymptomatic condition to persuade more men to be tested early.
When we hear about a disease, prostate cancer, or anything else, we naturally want to know what the symptoms are. How do we know we have it?
There are no warning signs for most patients with prostate cancer, especially those of us with low-risk prostate cancer
We may have urinary symptoms from enlarged prostates but that doesn’t necessarily translate into cancer.
Yet in the public mind, prostate cancer, even in those of us on active surveillance, is associated with lower urinary tract symptoms (LUTS)--such as frequent urination and pain while urinating or ejaculating.
The media often reports there are warnings that LUTS are an early warning for prostate cancer.
It is clear that prostatectomies can cause urinary problems such as incontinence, dispatching grown men into diapers.
Seemingly well-meaning consumer-oriented articles even by physicians and information on prostate cancer disseminated by hospitals and other organizations often stress LUTS in prostate cancer. As the British researchers said, this may be backfiring as men wait for urinary symptoms to emerge before getting checked out with screening.
Here’s an example of what’s going wrong from a hospital in Rhode Island (highlights added). (Note the disclaimers.)
What are 5 Common Warning Signs of Prostate Cancer?
In many cases, prostate cancer does not produce clear symptoms in its initial stages of development. In fact, many men may have prostate cancer without even realizing it.
However, there are some common warning signs that could indicate a person has prostate cancer.
Five of the most common ones include:
Pain and/or a "burning sensation" when urinating or ejaculating
Frequent urination, especially during the nighttime
Trouble starting urination, or stopping urination once in progress
Sudden erectile dysfunction
Blood in either urine or semen
Of course, these five symptoms are not the only potential warning signs of prostate cancer. Other possible indicators could include weak urine flow, and unexplained pain deep in the groin area when sitting down. (The prostate gland is located beneath the bladder and in front of the rectum.) If cancer has spread beyond the prostate, a man may also suffer lower body swelling, abnormal urinary or bowel habits, or inexplicable (possibly sudden) weight loss.
It's important to note that most of these symptoms are not unique to prostate cancer, and may indicate a different condition that is not life-threatening.
The hospital urges readers to get medical attention for these symptoms, which might be for prostate enlargement but not early-stage prostate cancer.
What Should You Do if You Have the Symptoms of Prostate Cancer?
If you are presenting one or more of the warning signs of prostate cancer, then it would be wise to promptly consult with a qualified physician. Your symptoms may indicate another, less serious condition; and even if you do receive a diagnosis of prostate cancer, it is much easier to treat this disease when detected early on.
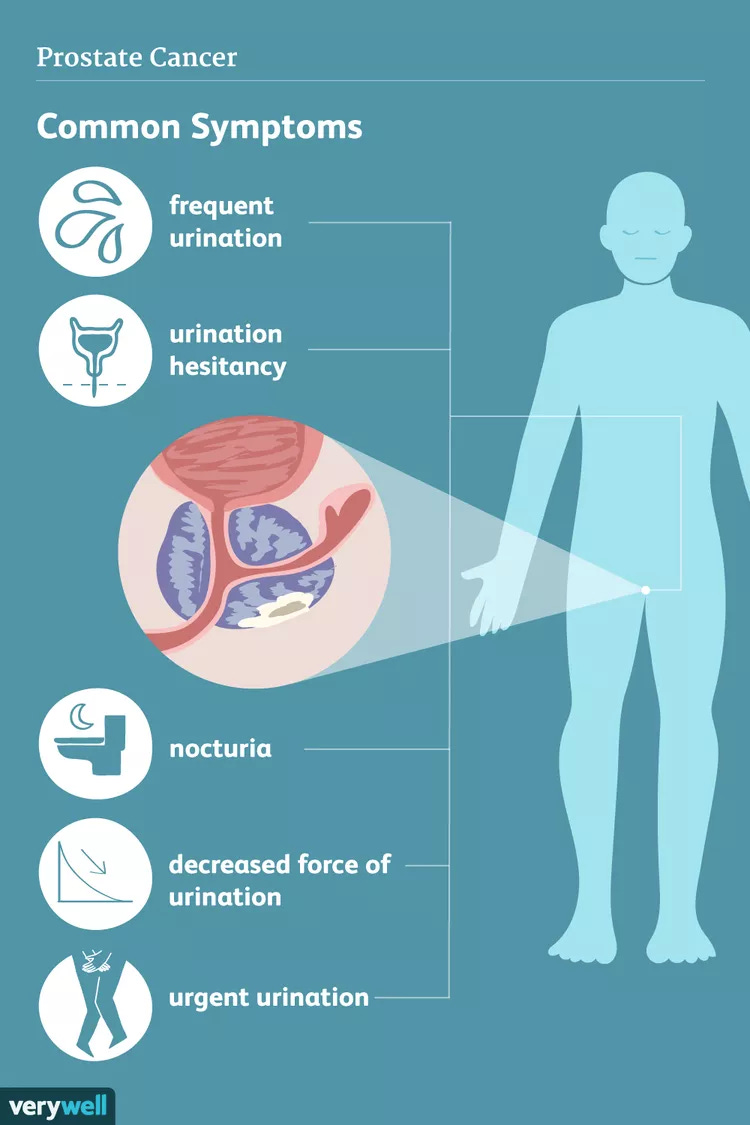
Now try this chart from an online consumer article by an MD.
Note the label: “Common symptoms.” Really?
The article also says: “Urinary frequency is one of the most common symptoms of prostate cancer. … Not only can prostate cancer lead to frequent urination, but it can cause a sense of urgency—the sensation of having to urinate right away. Men might notice that they need to walk rapidly to the bathroom or wonder if they will make it in time.”
Check out this guideline at Cancer.net from the American Society of Clinical Oncology.
It says there are usually no symptoms (highlights added) and then goes on to list them:
While most prostate cancer does not cause any symptoms at all, the symptoms and signs of prostate cancer may include:
Frequent urination
Weak or interrupted urine flow or the need to strain to empty the bladder
The urge to urinate frequently at night
Blood in the urine
New onset of erectile dysfunction
Pain or burning during urination, which is much less common
Discomfort or pain when sitting, caused by an enlarged prostate
So the message is getting out. But is it the right message?
Gnanapragasam and colleagues said:
Waiting for troublesome lower urinary tract symptoms as a trigger to see a GP about prostate cancer may potentially delay earlier diagnosis and management.
There is no evidence of a causal link between prostate cancer and either prostate size or troublesome male urinary symptoms. In fact, most evidence points to an inverse correlation.
Modern image-based diagnostics and risk-adapted management strategies have reduced the risks of over-investigation and over-treatment which previously deterred greater promotion of PSA testing in men with no symptoms.
It is now timely to re-brand early, curable prostate cancer as primarily an asymptomatic disease to encourage more men to come forward and get tested earlier.
The authors conclude: “If rates of earlier diagnosis are to improve, we call for strong clear messaging that prostate cancer is a silent disease especially in the curable stages and men should come forward for testing regardless of whether or not they have symptoms. This should be done in parallel with other ongoing efforts to raise awareness including targeting men at highest risk due to racial ancestry or family history. While the current resurgence in interest and debate about prostate cancer screening is timely, change of this message by guideline bodies, charities and the media can be a first simple step to improving earlier presentation and hence cures rates.”
Finish our AS survey.
We need your help.
Are you on Active Surveillance for low-risk Gleason 6 prostate cancer to favorable intermediate-risk prostate cancer? Or have you moved on from AS?
We need your help with a survey designed to determine patient views on AS. Data will be used to inform policymakers, guideline writers, and clinicians about where we stand on key issues.
For example: Will renaming Gleason 6 lesions as noncancerous reduce mental distress and financial toxicity in patients on AS? Should U.S. guideline writers, as their European counterparts did last year? favor safer transperineal biopsies vs. transrectal biopsies that can cause sepsis and other infections?
AnCan Virtual Support Group for Active Surveillance, Active Surveillance Patients International, Prostate Cancer Support Canada, and The Active Surveillor newsletter are asking for you to participate.
To participate in the survey, click here: https://www.surveymonkey.com/r/W69XXDS
Moving AS to the next level
By Howard Wolinsky
The Active Surveillance Coalition, a collaboration of leading support groups for active surveillance (AS) for prostate cancer, is sponsoring a webinar at 9 a.m. Vancouver/12 p.m. New York/5 p.m. London/6 p.m. Amsterdam on Thursday, Nov. 17 to discuss how we can move the needle on AS, close monitoring of prostate cancer.
AS leaders from Sweden, Holland, the United Kingdom, and the state of Michigan’s will share their “secret sauce” for reaching AS rates of near 90% and above.
The free webinar is entitled “Moving AS to the next level: Can we help more patients?”
Register here: https://bit.ly/ASnextlevel
The United States has lagged behind other wealthy countries in AS acceptance though the approach started here and in Canada in the late 1990s. AS uptake with AS finally reached a majority of 60% in 2021. The American Urological Association in 2022 set a new goal of 80% In 2010, only 6% of patients qualified for AS opted for this approach.
Several European countries and the state of Michigan’s MUSIC (Michigan Urological Surgery Improvement Collaborative) program have reached AS uptakes of around 90% or higher.
Panel members will present their stories followed by a discussion and a Q&A involving the audience.
The United States has lagged behind other wealthy countries in AS acceptance though the approach started here and in Canada in the late 1990s. AS uptake with AS finally reached a majority of 60% in 2021. The American Urological Association in 2022 set a new goal of 80% In 2010, only 6% of patients qualified for AS opted for this approach.
Several European countries and the state of Michigan’s MUSIC (Michigan Urological Surgery Improvement Collaborative) program have reached AS uptakes of around 90% or higher.
Panel members will present their stories followed by a discussion and a Q&A involving the audience.
AS 101 is a series of videos in which real patients and their partners ask experts about AS.
Active Surveillance 101 - Part 2 featuring Nancy and Larry White and Dr. Laurence Klotz at ASPI on Oct 29, 2022 12:00 PM Eastern.
Register at https://bit.ly/3SENBAd
To view session 1 go to https://bit.ly/3BUCxIE featuring Nancy and Larry White and Steve Spann, MD, family physician and dean of the University of Houston College of Medicine.