Glimpse into the future: Could proxy prostate cells in a dish replace biopsies in AS and test meds in advanced PCa?
My further adventures in Kidney Stone-land; Forbes' Millenson takes a look at PCa
By Howard Wolinsky
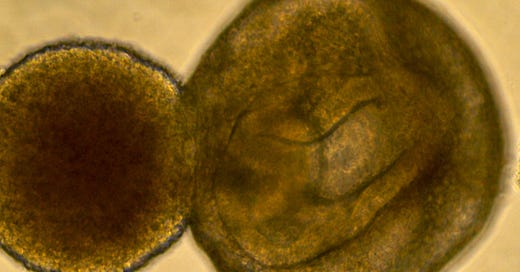
Picture this: Tiny prostate cells in a lab dish being used for cellular biopsies, sparing patients from being jabbed to extract cores and also eliminating the risk of sepsis. And how about developing the same proxy prostate cells from patients with more advanced cancer to see how effective drug therapy would be on them?
(Prostate cells made from stem cells at Cedars-Sinai.)
Researchers from the Cedars-Sinai Cancer Center and Regenerative Medicine Institute in Los Angeles and Northwestern University Feinberg School of Medicine in Chicago are developing these cellular models. Initially, they are recruiting men with prostate cancer who are positive for BRCA2, the inherited mutation associated with prostate cancer as well as breast, ovarian, and pancreatic cancer, melanoma, and other cancers.
Stem cell researcher Clive Svendsen, PhD, director of the Regenerative Medicine Institute at Cedars, said if this work is successful, the approach will be applied to stem cell research in men with all grades of prostate cancer, from active surveillance for low-risk disease to advanced, metastatic disease.
I have already raised my hand as a volunteer when that day comes.
(Clive Svendsen, PhD, director, Regenerative Medicine institute at Cedars-Sinai in LA.)
Svendsen is working with Dan Theodorescu MD, PhD, director of the Cedars-Sinai Cancer Center, a leading cancer researcher and an expert in functional genomics, and William Catalona, MD, professor of urology at Northwestern University Feinberg School of Medicine in Chicago, a pioneer in prostate-specific antigen (PSA) testing and nerve-sparing prostatectomy.
Over the past 15 years, researchers around the world have turned the genetic clock back on skin and blood cells to create embryolike cells, known as induced Pluripotent Stem (iPS) cells. iPS cells can be reprogrammed to become a wide variety of cells, including beta islet cells potentially to treat diabetes, blood cells free of cancer for leukemia patients, or neurons potentially to treat patients with neurological disorders.
Perhaps you have seen the video of a petri dish with individual synchronized heart cells?
In this case, the goal is to create patches to replace cardiac cells permanently damaged in heart attacks.
“The idea is to take iPS cells and make them into prostate cells, and then test them in the lab for their genetic and pharmacologic vulnerabilities. We've done this already with pilot samples,” said Theodorescu.
(Dan Theodorescu MD, PhD, director of the Cedars-Sinai Cancer Center
He said the group would then use pharmacologic and functional genomics approaches that he has developed to see which genes are driving BRCA2-mutation-containing cells are more prone to become prostate cancer in the dish and in animals, compared to patients who also have prostate cancer but don't have BRCA2 mutations or patients who never had prostate cancer.
“We're going to start with those because Clive has a large collection of iPSC from patients that have never had prostate cancer. That's the plan,” Theodorescu said.
Svendsen oversees “Answer ALS” – a set of 1000 iPSC lines for the production of a lethal neurological disease that is now being used to understand more about ALS.
The researchers hope to do the same type of study for prostate cancer. The first job is to generate miniature clumps known as organoids—roundish balls of cells that somewhat resemble prostate tissues, Svendsen said.
He said working with these cells “is like doing a biopsy, but without the pain. They’re actually identical to the patient’s prostate. The genetics are all identical between the iPS prostate cells and regular prostate cells.”
Svendsen, whose specialty is developing disease models, said they draw a blood sample to make iPS cells. They also could use a punch to take skin samples.
“The patients can be 80 years old, or 70 years old, or 60 years old. It doesn’t matter. We reprogram the cells. They go back in time to an embryonic state. And at that point, we can expand them forever. And those are the cells that can generate the beating cardiomyocytes, those famous beating cells. But we can also generate prostate tissue. So, the organoids grow after about three months in the petri dish, and they’re the same as your prostate.
“The beauty is, it's yours. The question I have is, in a man with prostate cancer, could we predict his prognosis from this organoid? Could he be a good candidate for surveillance, or should more aggressive therapy be carried out? And if we embark on surveillance, you wouldn't have to have a biopsy every year or two because we could say, you know what? We grew your prostate organoid, and it didn't grow aggressively—it was very slowly progressing in our model, whereas if it went really fast, we'd say, you know what? Go and have that prostatectomy as soon as possible.”
Theodorescu and Svendsen are an ideal team for this project. Theodorescu is a urologic oncologist, cancer biologist, and a leading researcher in functional genomics aimed at identifying tumor and metastasis drivers. Together, they bring expertise on iPS cells with that in genomics and prostate cancer to this project with the goal of enhancing the precision of cancer medicine for patients.
The National Cancer Institute defines precision or personalized medicine as “a form of medicine that uses information about a person’s own genes or proteins to prevent, diagnose, or treat disease. In cancer, precision medicine uses specific information about a person’s tumor to help make a diagnosis, plan treatment, find out how well treatment is working, or make a prognosis. Examples of precision medicine include using targeted therapies to treat specific types of cancer cells, such as HER2-positive breast cancer cells, or using tumor marker testing to help diagnose cancer.”
Theodorescu said, “The key for me is we can select the patients who you know have a specific genotype or prostate cancer and predict how they will do as well as treat them with specific drugs for them, rather than just throwing the kitchen sink at every patient that comes through the door.”
(William Catalona, MD, Northwestern University Feinberg School of Medicine, Chicago.)
Catalona, a key researcher on the project, is working with the LA team in recruiting patients for the study, including the sons of patients who have BRCA and prostate cancer. These subjects are aged 9 to 18.
The researchers want to see if the iPS cells generated from male children exhibit the same genetic predispositions as their fathers. About 10 patients have been recruited to date, with a goal of 50.
Svendsen said the pilot research involved prostate organoids developed from healthy men as well as men with prostate cancer.
The odds for success seem good. The researchers already showed in ovarian cancer that they could model the disease by making organoids from fallopian tube cells. The Telegraph reports here on this study.
The. researchers have grown a prostate cell from a patient with a BRCA2 mutation. “We have yet to see if they evolve into cancer. Studies are underway,” said Svendsen.
He added, “At the moment, we're in very early stages. We have grown prostate organoids from a few men with BRCA2 mutations and prostate cancer. So, we need to expand this to a larger number of patients and then show that this model works.”
He added, “We're on the edge of being able to combine this stem cell technology with functional genomics and ushering in a whole new era. I think we're going to look back in 10 years, and you're going to have your own prostate organoid floating around, saying you've got another 10 years, Buddy. You're good.”
[Patients who want to participate in this research should contact Catalona in Chicago at William.Catalona@nm.org , or Theodorescu at Dan.Theodorescu@cshs.org in LA]
(DreamStudio’s AI’s version of Picasso’s The Prostate.)
An update: My life as a kidney stoner
By Howard Wolinsky
I thought I got off easy. In the end, I didn't.
(Sensitive readers can stop here. This is meant for education and entertainment.)
My kidney stone was found by accident in a CT for another reason last fall. I had virtually no symptoms in the following months: Mild lower back pain.
I tried to wait it out. It didn't work. Drinking half of Lake Michigan wouldn't have washed away this little bastard., as it turns out.
(DreamStudio AI: Calcium oxalate stones on a stainless steel tray.)
The stone had a sharp tip that latched onto a spot halfway down the ureter, the tube connecting the kidney and bladder.
So they brought in the little guns last Thursday--a laser to break up the lone stone and a wire net to snatch and grab the fragments.
Again, I thought I got off easy.
After surgery, I had some tolerable urinary burning and brief ureter spasms along with blood in the urine and orange discoloration from one of the meds. I took a pain med and one for inflammation.
But the pain was mild and then gone minutes later.
Next step: the stent.
I got mixed messages from other stoners about removing a stent that kept things flowing.
Did it hurt? Didn't it? Depends on whom you ask—only your own experience counts.
I had the procedure on Monday. It wasn't bad--except when the stent seemed to get snagged. A nurse tugged on a string to pull out the device while I was on my back on an exam table with draping flashing the Full Monty.
All dignity goes out the window in these situations. I went with the flow.
Again, not that bad. Was I home free? I thought so. Wrong again.
Then, Monday night I experienced pain like none I had ever experienced previously. It would't let up. I started pacing and squirming. I couldn’t sit still.
I saw white. I couldn't focus.
I was disoriented.
(This pain chart just doesn’t do the job.)
(DreamStudio AI painting of pain by Picasso.)
I would register this pain a 20 on that 10-point scale for pain. The pain was beyond unimaginable.
It was phantom kidney stone pain WITHOUT a stone. I finally understood why women say that kidney stone pain is more intense than childbirth. A high school chum said she doesn’t remember the pain of childbirth, but will never forget the pain from kidney stones.
Looked like I had a midnight ER run in the cards.
But Judi reminded me I had taken some medicine for back pain. I stopped taking it because I had had a bad reaction.
But I dug up the meds and threw caution to the wind. This was an emergency.
So I gulped down the pill.. The pain let up, and I fell asleep in a matter of minutes.
Hallelujah.
I woke in the AM, feeling like I had been beaten up.
I spoke to the urologist.
No real explanation for what had happened. Dr. C. said I might have passed a blood clot. I don't think so. Maybe.
He said Judi had the right idea to take the back pain medicine. He re-upped my kidney pain med.
Tuesday, I had more pain but tolerable and took the kidney pain med. Wednesday, I felt like my kidney had been pummeled, but I didn’t have active pain.
So it goes.
(DreamStudio AI of kidney stone by Salvador Dali.)
In May, I have follow-up testing, a plain X-ray and ultrasound, to determine the state of my stones, if any, and develop a plan to avoid future stones.
The doctor says I'm not considered high-risk for stones--I've had a total of two since 2014. He said I need to drink lots of water and reduce salt.
Message received.
(Editor’s note: Mike Millenson, is my old friend—and competitor.
Mike was a medical writer at The Chicago Tribune. I was a medical writer “across the street” in those days at the Chicago Sun-Times. We each said the other worked for Brand X.
You might recall the Siskel and Ebert “At The Movies” competition. It was like that.
Mike was nominated for a Pulitzer three times. I am a two-time nominee (or loser, depending on how you view it).
Mike is still writing for Forbes but also is a medical consultant on the quality of medical care and is an adjunct associate professor at Northwestern University Feinberg School of Medicine. I’m still on faculty at NU’s famed Medill School of Journalism.
Below is Mike’s take on “good news” for patients with prostate cancer.)
Good News For Guys: “The Finger,” Your Sex Life And Prostate Cancer
Contributor
Forbes.com
Long before the Internet, “digital health” for men of a certain age meant the insertion of a gloved digit into your rear end by a urologist searching for early signs of prostate cancer.
Now, however, it may be time for some men to wave farewell to “the finger.” And in other good news, new evidence supports therapy for localized prostate cancer that avoids the risks of incontinence and impotence that have long haunted more aggressive treatments. Finally, announcements by two start-ups using artificial intelligence (AI) promise to improve diagnosis and treatment choice.
(Give it a read: full text.)
Mike ends his piece with some comments from me:
“Howard cautions, however, that choices for different individuals can still be confusing. “I don’t tell other men what to do. I just tell them what I’ve done,” he says.
Howard was diagnosed with early-stage prostate cancer in 2010, but despite six biopsies and more than 80 “core samples” from his prostate since then, only one very small cancerous sample has been found.
Of his 2010 diagnosis, he concludes, “I guess I just was having a bad prostate day.”
I like to get the last word in.
Question: Inquiring minds want to know: Do you wear a tie when you have a digital rectal exam? And are you on your back when it’s done? Please comment.