(Editor’s note: Jeff Coleman and I were emailing the other day about something or other, and he mentioned his “roller coaster of emotions” with having been diagnosed with perineural invasion. I published Jeff’s story on Sunday. I told him I coincidentally was preparing an article on PNI, featuring an interview with Hopkins urologic oncology fellow, Claire de la Calle, MD, who had reported on PNI in May at the American Urological Association annual meeting. Here’s Part II.)
By Howard Wolinsky
Invasion, in any context, is a scary, loaded word:
(1) The incursion of an army for conquest or plunder. Like the Russian invasion of Ukraine. Or Dr. Mark Scholz and Ralph Blum’s classic book, “Invasion of the Prostate Snatchers” about the prostate cancer-industrial complex.
And of course, the U.S. Congress for the first time in 50 years is holding hearings on those invaders of planet Earth, aliens, rather than those from Mexico and Central America. Our eyes are on the skies for an invading force, not some Latinx people seeking an escape from dangers back home.
(2) The incoming spread of something, usually harmful. Like the multiplication of microorganisms such as COVID-19 and other viruses, bacteria, and parasites that are not normally present within the body.
So what gives with “perineural invasion,” a term that crops up in maybe 10% of pathology reports with prostate cancer on biopsy.
I have encountered patients on active surveillance for low- to favorable intermediate-risk prostate cancer who already are scared of AS when they encounter perineural invasion in their pathology reports.
Generally, most often, PNI, as it’s called in the trade, is not a big deal--but it may be a warning of more serious prostate cancer lurking in the prostate.
Claire de la Calle, MD, who is doing her fellowship training in urologic oncology at Johns Hopkins, told me “It is a big deal in the sense that it should not be ignored as it might be a sign of unsampled higher grade disease but it does not exclude you from AS. It means that we probably should watch you more closely.”
She just presented a study at the annual meeting of the American Urological Association looking at PNI on biopsy, not PNI in the entire prostate after radical prostatectomy.
What is PNI?
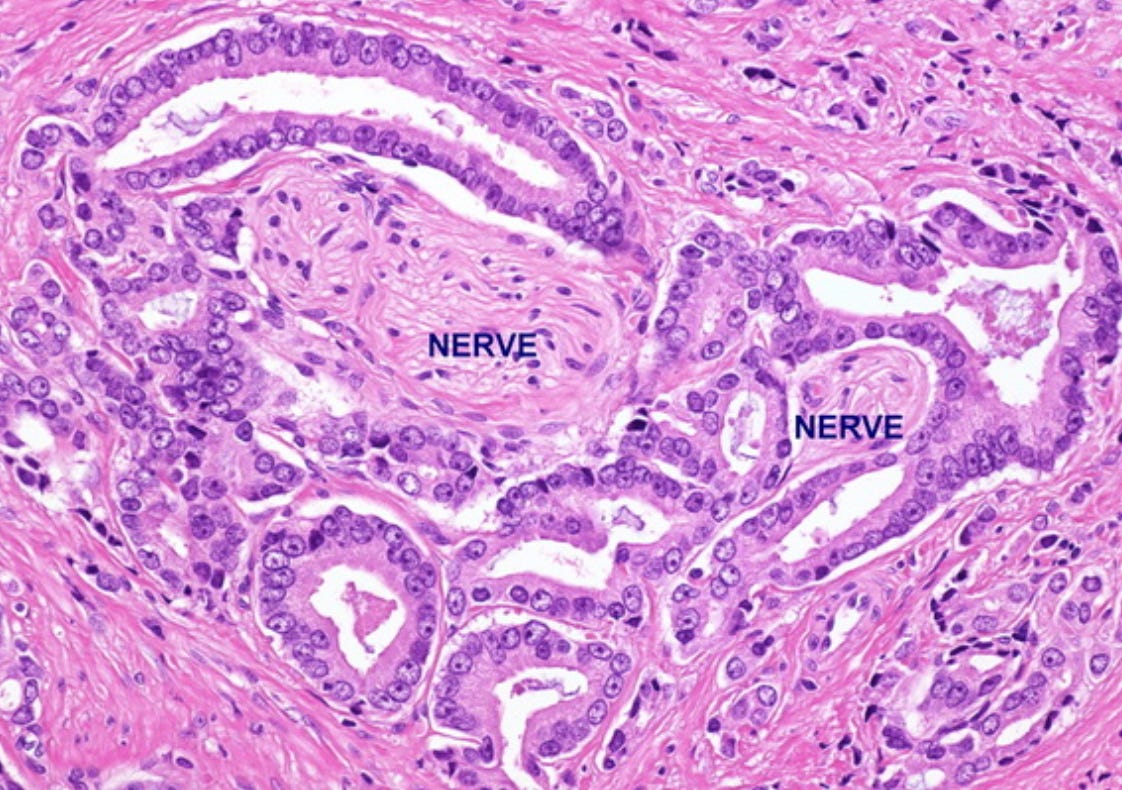
Perineural invasion simply means that cancer cells are found around nerve cells. Nerves are tubular structures with a sheath, which cancer cells can follow in a space between the nerve and the sheath. Think of a Trojan horse, or ants in single file following a scent path from the ground into your kitchen.
“Basically, perineural invasion means that there are cancer cells tracking along the nerve sheath. The prostate is an organ that is very innervated, meaning that there are a lot of nerves around the prostate and entering the prostate,” de la Calle said.
Perineural comes from Greek for peri (around) and neural (an adjective for nerves).
And don’t get perineural confused with transperineal biopsies, another animal altogether. The Latin means trans ( through) and perineal (an adjective referring to the perineum, the area between the scrotum and the anus.)
That’s the end of today’s lesson in etymology.
De la Calle said there is no standard definition of PNI in pathology. “Is it just a few cells? Does it have to be circumferential around the nerve or a little bit, so that’s just another factor that further complicates the equation,” she said.
(Claire de la Calle, MD)
And of course, the term scares the bejesus out of some patients who already are on anxious surveillance because they have been diagnosed with a Gleason 6--which sounds to some like death’s door, though it’s really the ground floor. In fact, a growing number of docs see it as a false cancer, a condition of aging that in most cases from which you won’t die.
(I recently co-authored a paper in the Journal of Clinical Oncology on the need to rename Gleason 6 as a non-cancer to reduce anxiety in part and also to reduce financial toxicity. (https://howardwolinsky.substack.com/p/extra-extra-read-all-about-it-renaming?s=w)
Several types of cancer, including prostate cancer, can exit organs and spread by using the nerves as a channel.
“In prostate cancer, it has been demonstrated that perineural invasion is a method by which the prostate cancer cells escape the capsule. That’s what we call extracapsular extension or extraprostatic extension.”
“It sounds like something pretty bad, right? The cancer is starting to progress and exit the prostate. However, sometimes, not commonly, we see perineural invasion in cancers that otherwise seem to be very low-grade, including in very low-risk prostate cancer patients with Gleason Grade 1 prostate cancer and otherwise very-low volume disease.”
De la Calle acknowledged it seems odd to find PNI with no other signs of a more clinically aggressive disease. She said researchers have looked into PNI as a potential predictor of something worse happening, such as a more aggressive cancer missed in a non-targeted, random biopsy.
Each biopsy we undergo for prostate cancer only takes a smidge of prostate cancer. Jonathan Epstein, MD, the prostate biopsy guru at Hopkins and a subscriber to TheActiveSurveillor.com, told me once that it would take 10,000 individual biopsies to get the full picture of a prostate. Just a “fun” fact, not gonna happen.
The other option is a radical prostatectomy--that’s really a sort of a joke. Those of us on active surveillance are trying to avoid biopsies.
De la Calle nodded in agreement: “Unless you remove the entire prostate from the body, you can’t know for sure that you don’t have unsampled higher grade disease. People have wondered if PNI is a sign of unsampled high-grade disease somewhere else in the prostate, or is it a sign of grade progression in the near future. People have looked at this in the past, but if you look at the literature, there are a lot of conflicting results.”
The problem is not in our stats. But it relates to this defect in biopsies: They seem to miss nerve samples.
De la Calle said, “We think that one of the reasons for these discrepant results is because not seeing PNI on a biopsy does not mean you do not have PNI. It can mean, you didn’t sample it, but also you have to sample nerves in the biopsy to be able to call PNI and it’s been shown that less than half of prostate biopsies even have nerves in the sample. We can’t see nerves on ultrasound, so it’s totally random if you were able to get some nerves or not. So, the pathologist isn’t even able to make the call if there are no nerves because you need to see the nerves to see if there is cancer going in them.”
Still, there are some potential concerns with PNI.
De la Calle said her research showed that patients with higher-volume Gleason Grade 1 tend to have more PNI than those with lower-volume Gleason Grade 1.
(She said the median maximum percent core involvement, was 10% in the patients with PNI versus only 5% in the men without PNI.)
“You always wonder if you see PNI, Is this a sign of unsampled higher-grade disease somewhere else in the prostate? The truth is you can never know for sure based only on the biopsy but you can only go based on the data you do have for sure. That’s why it’s still worthwhile doing an analysis of PNI,” she said.
She had some specific advice for those of us with very low-volume Gleason Grade Group 1, “We still had some patients that had very low-volume disease and PNI, and in those patients, the chance of reclassifying was even higher meaning in patients that have low-volume disease, the sign of PNI was an even stronger predictor In those patients we have a higher suspicion of unsampled either higher volume or higher grade disease.”
By the numbers
De la Calle’s group studied one of the world’s largest cohorts of patients on AS at Johns Hopkins. Researchers reviewed 1,969 of these patients in the Hopkins AS registry from 1995 to 2021. All patients had either very low-risk (n =1,282) or low-risk (n =687) disease at diagnosis and had at least one follow-up biopsy. They had a median age of 66 and a median PSA of 4.9 ng/mL.
During AS, the men with PNI had more grade classification to Gleason 7 and above (87 patients (43.9%) vs. 465 (26.3%), p <0.001), and were more likely to undergo any treatment than the men without PNI (120 patients (60.6%) vs. 667 (37.7%), p <0.001).
PNI was significantly associated with the reclassification of their Gleason scores. Sixty-three patients with PNI underwent radical prostatectomy (RP) (31.8%) vs. 390 men without PNI (22.0%) (p =0.003). The men with PNI had more extraprostatic extension at RP compared to the group of men without PNI detected at biopsy (33.3% vs. 19.5%, p =0.02), but there was no difference in other features of adverse pathology between the two groups.
Another opinion from a pathologist
Nancy Y. Greenland, MD, PhD, Assistant Professor, UCSF Department of Anatomic Pathology, and Staff Pathologist, San Francisco VA Medical Center, said reporting the PNI finding in prostate biopsy and prostatectomy reports is optional, de la Calle’s study adds to evidence supporting reporting it may be helpful.
“Most expert centers report on PNI routinely,” she said.
She observed that living with prostate cancer, even of the low-risk variety, seems challenging let alone being told you have an “invasion” of any sort.
She commented on my 12 years on AS and my efforts to have the cancer label removed from a Gleason 6 diagnosis.
She said: “I can imagine it must be stressful having a diagnosis of prostate cancer hanging over your head for that long and hence the motivation for cutting back on loaded words like ‘cancer” and “invasion.” Our pathological diagnoses are meant to be accurate and specific and so we rely on clinicians and educational materials (like yours) to help people know what to worry about and what is unlikely to affect their lives. As I mentioned, reporting of PNI is optional, but at UCSF and the SF VA we are careful to note it on all cases. The key finding of Claire’s study is that men with PNI deserve more close attention during active surveillance.”
The bottom line?
PNI detected on biopsy in patients with low-risk PCa on AS is strongly associated with grade reclassification, an increase in your Gleason score.
PNI should not preclude low-risk patients from being on AS but, de la Calle said the findings will allow urologists to better counsel men with PNI in choosing AS versus treatment and help determine how aggressively to monitor these patients while on AS.
TheActiveSurveillor.com take-homes: It can be hard to learn to coexist with Gleason 6 indolent cancers. Likewise, PNIs can add to the upset. Remain calm, if you’re committed to AS, keep monitoring your cancer, and act accordingly.
PNI at WebPathology: “A cluster of malignant glands surrounds two nerve twigs. The role of perineural invasion as a prognostic indicator is controversial. There is conflicting data regarding its utility as a predictor of progression after surgery or radiation therapy. Since some clinicians use it in their treatment decisions, pathologists should document its presence in pathology reports.”
Time’s up here. Register STAT:
Two experts who have made big news on lifestyle and prostate cancer will share their research on diet, including plant-based and Mediterranean plus other lifestyle choices, including exercise and sleep, at an AnCan webinar for all patients with prostate cancer 8-9:30 p.m. Eastern on May 31.
Register: https://bit.ly/3KkxcfC
The webinar, entitled “Optimizing Sleep, Exercise, and Nutrition in Prostate Cancer," features Dr. Stacy Loeb, professor of Urology and Population Health at the New York University School of Medicine and the Manhattan Veterans Affairs Medical Center, and Dr. Justin Gregg, assistant professor of Urology and Health Disparities Research at UT MD Anderson Cancer Center, of UT MD Anderson Cancer Center in Houston.
Active Surveillance Patients International and the AnCan Virtual Support Group for AS are teaming up for a program on BPH (benign prostate hyperplasia), an enlarged prostate, a not uncommon problem in patients on AS with intact prostates. Men who have been treated encounter similar issues,
It’s a drop-in First Wednesday meeting, June 1 at 8 p.m. EST. No registration is necessary. Attend the free program, featuring BPH guru, Mount Sinai’s Dr. Steven Kaplan.
Just enter the AnCan Barniskis Room. And bring your questions .... in fact, if you already have something in mind, send it ahead of time to Joe Gallo at joeg@ancan.org.
Mark this on your calendar: Join me June 7 on Zoom at the Tri-Cities Support Group from outside Vancouver. I will nag you until you sign up. So sign up. Resistance is futile.
No registration necessary. Go to: https://bit.ly/3NGQQob
Here’s what Dale Bryant from Tri-Cities and Richelle Green from ProstateSupport Canada put together:
“Lessons Learned: My Prostate Cancer—and Yours”
JUNE 7TH, 2022 |
7:00 PM Pacific/8:00 PM Mountain/ 9:00 PM Central/10:00 PM Eastern
Go to: https://bit.ly/3NGQQob
The Tri-Cities Support Group's speaker will be Howard Wolinsky, a co-founder of Active Surveillance Patients International. Howard is an award-winning medical and science journalist from Chicago, who wrote for the Chicago Sun-Times. He recently started writing a newsletter: TheActiveSurveillor.com
Howard is the author or co-author of three books about medical issues.
Since he has been so willing to speak to people and write about his experience with prostate cancer, he is an ideal choice to introduce the topic of how to talk about prostate cancer to family, friends and those with whom we come in contact. We are hoping that his talk will serve as a springboard for an interesting sharing of information on how comfortable people are to talk about their prostate cancer journey with others.






Like the bogus microscopic determination of the G6 as a cancer, there is no hard scientific data that PNI is potentially deadly. Worse still, there is no hard scientific data to support surveillance biopsies randomly and blindly sampling 0.1% of the prostate as being safe and beneficial. The prostate cancer arena remains full of half-truths and misrepresentations and is mostly, without the support of irrefutable and reproducible data.
It was a few years ago that I read the book, this was when Ralph was first up at bat. I do believe the whole idea was his and that he corralled Dr. S. to go along with it. Which he was only too happy to do, of course. Not sure if it should be required reading for anybody who gets a PCa diagnosis, but as my grandmother (or someone's) used to say: It vudn't hoit.