The COVID-19 virus mistaken (initially) for rapidly advancing prostate cancer
Beware of COVID: A cautionary PCa tale.
By Howard Wolinsky
My old friend and fellow Active Surveillor David King Keller, PhD, of Jacksonville, Florida, noticed something strange going on: His PSA jumped 2 points in a short time. In addition, he experienced unexplained searing bone pain.
What does that sound like? The obvious? It seemed as though David was experiencing a dangerous turn in his prostate cancer.
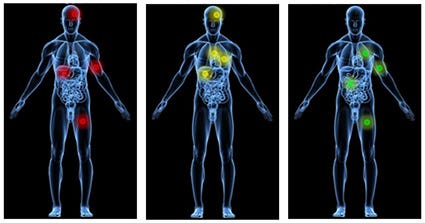
(Not this: Prostate cancer mets.)
“If a patient's prostate-specific antigen (PSA) spikes 2 points in just 90 days, what is your first thought? This patient has a strong likelihood of aggressive prostate cancer, right? If that same patient also presents with severe, burning bone pain with no precipitating trauma to the area and rest and over-the-counter painkillers are not helping, you'd think, ‘check for metastases,’ right?
“That patient was me in late January 2023,” David writes in Medscape.
But David is an intrepid researcher. He put his mad skills to good use once again.
He dug deep and found he wasn’t having a rapid progression of prostate cancer. He linked his symptoms to a simpler, very timely cause: COVID-19.
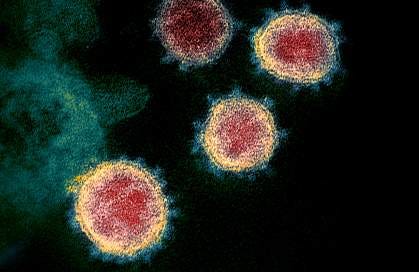
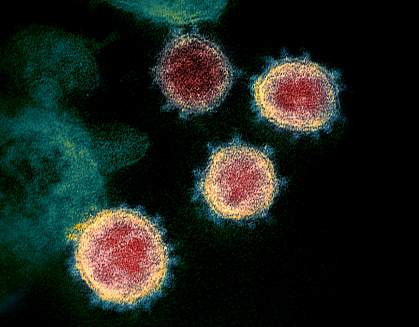
(This: COVID-19.)
He found a Turkish study showing that COVID itself can spike PSA temporarily for up to six months. He communicated with the authors using Google Turkish.
He explains in the article how one can have “burning bone pain without a precipitating trauma and why it should not be pre-judged as metastasis of one’s prostate cancer. This article is for every man with and without a prostate and for every man to send a link to his urologist and primary care provider,” he said.
Way to go, David.
Wish me luck in the OR Thursday: Stuck in the Middle…Again
By Howard Wolinsky
Clowns to left of me. Jokers to the right.
Here I am: I'm stuck in the middle. Again.
Something ain't right? Damn right.
I’m not talking about the 1972 hit song with the simulated Bob Dylan sound.
But I am talking about a freakin' kidney stone. Stuck halfway down the left ureter.
It’s only 4 millimeters--small enough to pass. But the little bastard is stuck halfway, about 11 centimeters down the tube.
So close. But not close enough to the exit. It just hasn’t budged since it was discovered by accident--in a CT for another reason--five months ago.
Initially, there were no symptoms. Then, I started having some lower back pain. IUt brought me back to summer 2014 when I previously had a kidney stone surgically removed.
This time around, I increased my water intake, which relieved the back symptoms but did nothing to move the stubborn stone.
Some stones are smooth. I suspect mine is different, that it armed with wings that allowed it to dig in.
My local urologist said lithotripy is out because of the stone's location. A famed Norwegian urologist told me it’s easier to shatter stones contained within the kidney proper.
He also told me a fun fact: Men are able to pass stones up to 4 millimeters, and women can pass them up to 6 millimeters. Go ladies, go.
Another fun fact from my transcriptionist who describes herself as a “stoner,” someone prone to kidney stones. She has given birth to two kids and dealt with multiple kidney stones, and, she says, the stones are worse.
I have been lucky my symptoms have been minimal, or maybe I am tougher than I had thought.
Three follow-up CTs found the stone was gathering no moss but could grow larger and shut down my left kidney. Not urologist-recommended.
I did my best drinking water, and eating cranberries. Folks, remedies ain't working.
I had one last Hail Mary CT on Saturday. But the stone is unmoved. It ain't goin' nowhere unless it is forced to.
So I am having surgery on Thursday.
My main concern? The last time I did this at UChicago, I ended up with low-grade sepsis. High fever, headache, punky feeling. Not good.
The surgeon, this time, promises no sepsis and no catheters. Hope so. Stay tuned.
ASPI takes on genetic counseling in AS 101—still time to sign up
By Howard Wolinsky
ASPI is premiering two segments of the AS 101 series aimed at educating patients about genetic counseling and Active Surveillance (AS).
The free program will be at 12 p.m. Eastern, Saturday, March 25. Click to register.
A Q&A session will follow the videos.
AS 101, like an introductory college course, was launched in 2022 to explain in short video chats the basics of active surveillance for the newly diagnosed, those in the “gray zone” with rising PSAs but no biopsy confirming the presence of low-risk cancer, and also patients who have been on AS for a while but are looking for a refresher course.
Each session features prostate cancer patient, Larry White, and his well-informed wife, Nancy White, speaking with top experts about questions they have about AS issues in an office visit setting.
(Justin Lorentz, genetic counselor.)
The Whites discuss genetics and genomics from a patient point of view with Justin Lorentz, MSc, a certified genetic counselor and lead of Sunnybrook Health Science Centre’s Male Oncology Research and Education (MORE) Program, a registry for men with hereditary cancer. Lorentz, who is an instructor at the University of Toronto, is also a consultant to the Promise study, which offers free DNA testing to U.S. men with prostate cancer.
***
The full series to date of AS 101 is available at: https://aspatients.org/a-s-101/
Episode 1. “Rising PSA,” featured Dr. Stephen Spann, a family doctor and founding dean of the University of Houston College of Medicine, who recommended that Larry, who has a rising PSA blood level, and his wife, Nancy, see a urologist.
Episode 2. “The Urologist” focuses on the Whites’ first visit with a urologist, Dr. Laurence Klotz, of the University of Toronto, the father of active surveillance.
Episode 3. “Active Surveillance.” Dr. Klotz recommends Active Surveillance for Larry White.
Episodes 4 & 5, “Counseling Before DNA Testing” and “Genetic Results.” The video focuses on Larry White’s inherited DNA to determine if he needs to take special steps.
Additional programs are coming with uropathologist Dr. Jonathan Epstein, of Johns Hopkins, on biopsies and Dr. Andreas Correa, of Fox Chase Cancer Center, on imaging prostate cancer.
AS 101 is a project of the AS Coalition, which includes ASPI, the AS Virtual Support Group from AnCan, the Prostate Cancer Research Institute, Prostate Cancer Support Canada, and TheActiveSurveillor.com newsletter.
Special thanks to Alex and Peter Scholz and their team at PCRI, who recorded and edited the program.
The Prostate Cancer Research Institute is holding the virtual version of its mid-year meeting on Saturday March 25 at 8:30 a.m. Pacific.
Register here.
These sessions are focused on more advanced prostate cancer. But patients with low-risk prostate cancer may find the session on PSMA PET scanning of interest, though this technology is not yet available to us. Also, the Q&A with Drs. Mark Scholz and Mark Moyad are always worth attending.
Check out Gleasson 3+4 patient Richard May’s experience with PSMA PET:
VIRTUAL | SATURDAY, MARCH 25, 2023 (Pacific Time)
8:30am - 9:00am / Mark Moyad, MD, MPH / Opening Remarks
9:00am - 11:00am / Advanced Prostate Cancer Treatments / Elisabeth Heath, MD
11:00am - 12:30pm / Prostate Cancer Imaging / Johannes Czernin, MD
12:30pm - 1:00pm / Lunch Session with Matthew Rettig, MD
1:00pm - 3:00pm / Proton Therapy / Carl Rossi, MD
3:00pm - 4:30pm / Q+A / Mark Moyad, MD + Mark Scholz, MD
4:30pm - 4:45pm / Closing Remarks
PCRI in September will focus on AS.



Thanks for the private messages re my impending surgery.
One reader mentioned he hoped I wouldn't need a catheter.
Me, too.
Last time, I had a catheter. This time they say none probably is needed. We'll see.
Might have a stent.
Last time, I had to extract the the catheter. I wasn't prepared for that. Once you start, you can't stop. It was freakishly long.
My new urologist said when he trained at Mayo Clinic, they sent patients home with catheters that they extract themselves. Now he's in private patients and has learned that patients hate that.
Thanks for asking, Steve.
Howard
Interesting. My first PSA result post-COVID was over 8, when the previous test had been just under 4. We did a round of antibiotics and it dropped to 4.5 in about 2 weeks. Glad we used antibiotics instead of a biopsy!