This just in: Researchers in prostate cancer and breast cancer surgery team up to promote Active Surveillance
Powerful op/ed in New York Times.
(New York Times guest essay on AS and prostate and breast cancer.)
By Howard Wolinsky
Breast cancer in women and prostate cancer men have a lot in common in terms of incidence, death rates, and the spectrum of disease from very low-risk to very high risk. And in their low-risk forms, both can qualify for Active Surveillance, though the approach, thus far, has been more successful in men than in women..
Dr. Laura Esserman, a breast cancer surgeon and researcher at the University of California, San Francisco, and Dr. Scott Eggener, a prostate cancer surgeon and researcher at the University of Chicago, [call them E-squared] for more than a decade have been making the case that the low-risk versions of these cancers can be safely monitored, that there need not be a rush to aggressive treatment with surgery or radiation.
They’re at it again in a guest essay in today’s New York Times. It is a must-read, whatever your position on this issue.
In particular, the debate on renaming Gleason 6 has been simmering. The addition of the breast cancer side adds more power and weight to the discussion.
E-squared said: “We are oncologists with expertise in prostate and breast cancers. We believe the medical community must reconsider what we call cancer in its earliest manifestations. So do a growing number of cancer experts around the world.”
(Dr. Laura Esserman on the right.)
“Early detection of cancer sounds intuitively attractive and, in many cases ,saves lives. But automatically calling something cancer can lead to aggressive treatment, even if the cancer in question is unlikely to cause problems. For many cancers, the term simply doesn’t match how the disease behaves.”
“As cancer surgeons, knowing what we now know, we wish we could go back and undiagnose or reclassify a significant proportion of our patients,” they add with remarkable candor.
Wow.
(Dr. Scott Eggener on the right.)
Eggener, my former urologist, saved my bacon—and prostate—in 2010 when he told me I was the “poster boy for active surveillance.” He got it right. In fact, the initially diagnosed cancer was never seen again in five other biopsies.
I had a single core of what’s been called a “wimpy” cancer out of more than 80 cores. And then it disappears. I have heard similar stories from several other men. You call that cancer?
In 2010, a urological surgeon I call the “Notorious RP” tried to sweettalk me into an OR to “cure” my cancer. Back then, he told me he didn’t support AS—though I understand that he does now.
This debate is not new, but it is gaining momentum. I wrote about it in Chicago Medicine Magazine in 2013 just three years after being diagnosed and put on AS.
(My article from 2013 in Chicago Medicine)
I took another look in my MedPage Today blog, “Is This Really Cancer?—Movement builds to classify Gleason 6 prostate lesions” as Eggener launched a campaign to rename prostate 2021.
There’s been pushback as about 50% of urologists and 90% of pathologists oppose any change, arguing that men will drop AS and put themselves in jeopardy if the cancer label were dropped. Not all patients agtee either.
There has been considerable discussion as demonstrated when an article,”Low-Grade Prostate Cancer: Time to Stop Calling It Cancer,” led by Eggener in which several physicians and I were co-authors, was the best-read article in the Journal of Clinical Oncology in 2022.
Today, Eggener and Esserman (E-squared) are making the case that some things we call cancer may not actually be cancer.
E-squared estimate that 20 percent to 25 percent of prostate and breast cancer diagnoses—about 100,000 patients a year—in the United States are low risk and can be managed with observation. “These patients are routinely treated with surgery or radiation, even though their conditions are not life-threatening and cause no symptoms at the time they are spotted. To our knowledge, neither Gleason 6 nor D.C.I.S. spreads to other parts of the body unless more aggressive forms of cancer develop or are simultaneously present. They are more accurately explained as risk factors for prostate or breast cancers with malignant potential,” the researchers said.
Active surveillance—close monitoring— has taken off among men internationally. Most men want to hold onto their prostates and avoid erectile disorder and urinary and fecal incontinence caused by aggressive treatment.
About 60% of American men with low-risk Gleason 6 prostate cancer opt for AS. That’s not bad compared to the 6-10% who went on AS in 2010. But that’s far below the 90%+ achieved in Michigan, Sweden, and the United Kingdom.
AS used to be a hard sell. The idea seems crazy, that a cancer is diagnosed and then you do nothing but monitor it.
But researchers have been building an impressive arsenal of research making the case for AS. Likewise, patient advocates and support groups only focused on AS have been a success.
Talk about a hard sell? Women, who are more health conscious to begin with, are not buying this concept in breast cancer, no matter how low-risk their cancer may be. AS is a non-starter though Esserman and others are launching clinical trials that may help clear a path.
Last year, Esserman invited me to partner with and advise her group on AS in a screening trial for breast cancer called WISDOM. She told me that as many as 60% of women can qualify for AS for breast cancer.
She faces obstacles in pulling this off as patients and their families are resistant.
Esserman recently told me: “When you look at breast cancer, nobody's doing active surveillance, even for the really low-risk, low-grade cancers. We can barely get people to do it for D.C.I.S.”
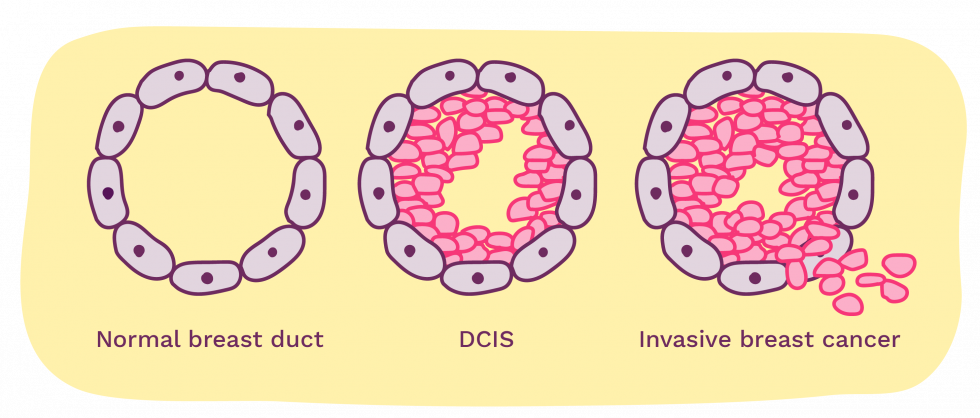
D.C.I.S is shortductal carcinoma in situ, the presence of abnormal cells inside a milk duct in the breast. “DCIS is considered the earliest form of breast cancer. DCIS is noninvasive, meaning it hasn't spread out of the milk duct and has a low risk of becoming invasive,” according to the Mayo Clinic.
Sound familiar to you? Almost like low-risk Gleason 6 (Grade Group 1) prostate cancer.
The researchers make the pitch for renaming these “cancers” to reduce emotional distress and financial toxicity, such as problems getting insurance and advancing on the job because you have “the Big C,” no matter how small that C actually may be.
E-squared said: “Renaming very low-risk cancers would make it easier to persuade patients when it’s appropriate to adopt monitoring and risk reduction as their approaches. Early-stage ‘cancers’ that meet the microscopic definition of the disease (what a pathologist sees through the microscope) but not the clinical definition (a condition that is highly likely to grow and cause symptoms and has the potential to kill a person) could be designated as IDLE (indolent lesion of epithelial origin) or preneoplasia — anything but the dreaded C-word.”
The rename game has been played successfully for certain thyroid, bladder, kidney, and cervical cancers. Even Gleason 5 used to be considered cancer. This change could happen.
The researchers said: “Clinical surveillance studies in Gleason 6 prostate cancer have shown that this approach has reduced overtreatment substantially. For D.C.I.S., a majority of hormone-positive patients — in which cancer cells contain certain proteins that can be targeted to reduce the chance of cancer arising — may be suitable for active surveillance with therapies to slow or stop the growth of hormone-sensitive tumors, but we won’t know until we study it. Perhaps most important, D.C.I.S. may offer a window to study preventive or risk-reducing interventions.”
(I wonder if that truly would be AS. But we can talk about that another day.)
(https://breastcancernow.org/information-support/facing-breast-cancer/diagnosed-breast-cancer/primary-breast-cancer/ductal-carcinoma-in-situ-dcis)
D.C.I.S. ought to follow the lead of AS in low-risk prostate cancer and save women from unnecessary and aggressive treatment.
Tick-tock: Join trailblazing researcher Dr. Laurence Klotz in a webinar on focal therapy on Aug. 31
Dr. Laurence Klotz, of the University of Toronto, one of the fathers of active surveillance, also is a pioneer in focal therapy, methods to remove lesions without performing radical prostatectomies.
He will share his experience in a free webinar at 8-9:30 p.m. August 31 entitled, "Is focal therapy right for your prostate cancer?" Register at https://attendee.gotowebinar.com/register/1495697985984134744
Send questions in advance to Joe Gallo at joeg@ancan.org. (Happy Birthday, Joe.)
You should leave the program with an understanding of whether you are a candidate—or not—for focal therapy. FT’s not for everyone.
Focal therapy offers middle-ground therapy for men with localized prostate cancer. It uses ablation, or tissue destruction, to target the area that contains the index lesion. Men who have focal therapy will continue to be monitored after treatment.
This program is aimed at the newly diagnosed who are considering options and those who are considering leaving Active Surveillance.
If you can’t make it, register, and you’ll automatically get the link to the video link.
Laughing your prostate off in the Gleason awards—deadline extended
By Howard Wolinsky
Submit your prostate jokes, cartoons, limericks, whatever—on DREs, PSAs, BPH, and prostatitis—to The Gleasons—Putting The Glee In Gleason Scores, the first prostate humor contest.
The contest, started by Jim-Bob Williams, a therapeutic humorist and Gleason 6 patient, and me, is open to doctors and patients alike. The deadline has been extended to Sept. 15 to help out some stragglers.
Share your prostate humor at howard.wolinsky@gmail.com Jokes, limericks, poems, whatever floats your boat. We do play blue so ED and Viagra jokes are in play.
A distinguished panel will announce the winners later in September, Prostate Cancer Awareness Month.
(Sir Billy.)
In the professional division, AnCan Foundation has nominated Sir Billy Connolly’s over-the-top prostate exam bit: https://ancan.org/billy-connolly-prostate-examination/
Guaranteed that you’ll laugh your prostate—and ass—off.
Active Surveillance Patient International Sept. 30 webinar on lifestyle and low-risk PCa
By Howard Wolinsky
During September's Prostate Cancer Awareness Month, Active Surveillance Patients International (ASPI) sponsors a free webinar on lifestyle research and low-risk prostate cancer from 12-1:30 p.m. Eastern, Saturday Sept. 30.
Register here for “Applied Research and Lifestyles and Low-Risk Prostate Cancer," for: https://zoom.us/meeting/register/tJwvdOGoqjwuE9CC8AI45nYdsj63e-iUnop6
(Dr. Stacey Kenfield, on right, & Dr. June Chan, working out. Mario Sanchez UCSF.)
The program focuses on how men can take some control over their lifestyle, including eating, exercise, and exposure to known carcinogens. The program also will cover how mental health behavior may help the patient adhere to a healthy lifestyle. Please submit any questions ahead of the program to: contactus@aspatients.org.
The program includes:
—Dr. June Chan, of UCSF, on “The Role of Exercise for Deterring Prostate Cancer Progression/Death”;
—Dr. Stacey Kenfield, of UCSF, on “The Role of Diet for Men Living with Prostate Cancer”;
—Chan on “Lifestyle Scores & Prostate Cancer Progression”;
—UCSF dietitician Greta Macaire on “Practical Advice on Diet for Men Living with Prostate Cancer”;
(UCSF dietitian Greta Macaire)
—PA-C Christina Nakamoto, Medical Science Liaison for Urology at Myriad Genetics Inc., will cover cancer causes, such as carcinogens/diet/ hereditary, and mental health mindfulness for cancer.