Tipping the 'seesaw' on PCa screening in the UK
Still, U.S. lags on adopting safer transperineal biopsies
(Editor’s note: AnCan AS moderator Joe Gallo and I are holding a virtual support group for patients on AS at 10 a.m. Eastern on Monday, Feb. 27, during the ZERO Summit. Join the session via ZOOM at https://bit.ly/3HQl4Ux There is NO registration. So jot down that URL. Please join us.
By Howard Wolinsky
Britain has been slow to adopt screening with prostate-specific antigen (PSA) blood levels for fear that men will be harmed.
In fact, British patients must request PSA testing. But Britain has led the way in the use of MRIs to avoid biopsies and adoption of transperineal biopsies to prevent infection.
Researchers from Prostate Cancer UK found that 67% fewer men experienced harm from screening than in the past.
Their poster, presented last week at the American Society of Clinical Oncology meeting in San Francisco, is entitled, “Tipping the Seesaw.” The PC UK researchers said the “seesaw has certainly tipped by these harm reductions.”
(Note: Posters are not peer-reviewed.)
The researchers said in the past: “Screening for prostate cancer has been and remains contentious with evidence of harms and benefits finely balanced and inadequate to tip the see-saw one way or another in order to give men clear, understandable guidance on PSA testing.
Dr. Matthew Hobbs, lead author and director of research at Prostate Cancer UK, said: “We’ve known for some time now that testing more men reduces prostate cancer deaths, but there have always been concerns about how many men would be harmed to achieve this.”
But things have changed in the UK anyway.
“In recent years, the diagnostic pathway has changed significantly, delivering a modern pathway that is likely to do far less harm and possibly more benefit. Our work quantifies the levels of harm and benefit at each stage of the entire pathway currently used in the UK from initial PSA through to biopsy-confirmed diagnosis of prostate cancer.”
The authors found for every 10,000 men who had a PSA test, 463 would be diagnosed with a clinically significant localized prostate cancer, 110 would be diagnosed with a clinically insignificant prostate cancer, and 646 would go through the entire diagnostic pathway with no diagnosis of prostate cancer.
They said a “maximum” of 38 men would suffer clinical side effects from a biopsy.
“Rates of biopsy-related harm in modern practice are encouragingly low and likely to reduce further,” researchers said.
(True in the UK—not in the USA. See more below.)
Unlike the U.S., Britain, in recent years, has adopted safer transperineal biopsies that prevent virtually all sepsis and other infections because they have replaced transrectal biopsies, which involve needles passing through the germy rectum into the prostate.”
The UK National Screening Committee is scheduled to re-examine prostate cancer screening.
The researchers concluded: “Rates of biopsy-related harm in modern practice are encouragingly low and likely to reduce further. A PSA-initiated diagnostic pathway misses a significant proportion of clinically important cancers. It is interesting to note the high conversion from MRI to biopsy in the data underpinning this model. Next steps will include analysis of the same outcomes in several centers in the UK to determine if actual practice matches expected outcomes (harms and benefits) from previous clinical trials.
In response to the study, Ros Eeles, Professor of Oncogenetics at The Institute of Cancer Research, London and Honorary Consultant at The Royal Marsden NHS Trust, said: “The study shows very interesting data which support the shift towards the investigation of how to implement prostate screening. European studies of using the blood marker PSA to direct screening have shown a reduction in mortality, but the concern has been overdiagnosis, including detection of some cases which would never have caused harm, and potential harms of overtreatment.”
Eeles added: “However, we know that about a quarter of cases will be aggressive and cause deaths. There is, therefore a need to identify techniques that will tip the balance of screening from risk to benefit. This useful study has looked at the use of MRI imaging and biopsy techniques which have a lower risk of infection and are showing promise in this area. It shows us a rationale for the way forward to implementing a prostate screening programme in the UK. The challenge will be to find better markers which indicate the presence of aggressive disease and to refine our use of genetic risk stratification to be able to target new methods of screening to those at highest risk. Our team’s research is investigating the role of genetic tests which can better risk stratify populations to target such screening programs.”
Britain and the rest of Europe have lagged behind the U.S. in use of genetic testing.
Back in the USA: Is Big Urology ready for reform? Don’t hold your breath.
By Howard Wolinsky
Across the pond, unfortunately, American urology has lagged behind UK and the rest of Europe in adoption of transperineal biopsies—to the detriment of patients like us who at risk—small but real—of potentially disabling and deadly sepsis.
Hein van Poppel, MD, adjunct secretary general and policy guru of the European Association of Urology, recently told me that in Europe transrectal biopsies are considered “medical malpractice.” In 2021, the EAU made transperineal biopsies the recommended approach.
Here in the USA, the land of baseball, apple pie, Chevrolet, and toxic transrectal biopsies, it’s the same old, same old—transrectal biopsies rule the day. Change is coming slowly.
Many patients are voting with their feet—and prostates. Trying anyway.
I hear nearly daily from men desperately seeking urologists trained to perform transperineal biopsies. Some travel 1,000 miles or more to have safer biopsies. But a minority of urologists are trained to perform modern transperineal procedures,
The latest numbers show that only 5% of American AS patients undergo transperineal biopsies. Our patient surveys going back to 2021 show that educated patients attending support groups, such as AnCan and ASPI, are far more likely to get TP biopsies than the general population who undergoes prostate biopsies.
The American Urological Association later this year will announce at its annual meeting in Chicago new guidelines regarding transperineal vs. transrectial biopsies.
Will AUA go the way of EAU?
Don’t hold your breath.
Big Urology ain’t necessarily ready for reform or looking out for patient interests.
The transrectal house is burning. But the AUA is waiting to be sure before calling the fire brigade.
There is a lot of doctor resistance to this change. There are reimbursement and retraining issues involved. It costs $40k for a urologist to set up TP in his or her office, plus it requires some time off to be retrained.
There are now no financial incentives for change. Reimbursement for urologists is the same whether they go with transperineal or transrectal biopsies, even though transperineal procedures take a bit longer. Changing reimbursement codes is akin to turning aircraft carriers.
In contrast, Australian uros, thanks to patient pressure, who are using transperineal procedures get double the fees of their colleagues performing transrectal biopsies. Money talks if given the chance.
I’m not persuaded that Big Urology thinks it has a problem even as some men quietly are dying and being disabled from sepsis that could have been avoided.
Check out my 2021 story, “No More Men Need to Die From Transrectal Prostate Biopsies— A movement toward transperineal biopsies” on this debate in MedPageToday
Based on Norwegian figures, one in 1,000 men die from transrectal biopsies. This translates to roughly 2,000 American men per year. Many American urologists are in denial—men may die a month or so after a transrectal biopsy—and urologists reflexively will say they have low sepsis rates in their practices.
Also, check out TheActiveSurveillor.com on this debate amongst U.S. urologists: “Great Biopsy Debate': Is 'Big Urology' ready for biopsy reform?” Please view the AnCan debate and reach your own conclusions.
While you’re at it, why not sign my petition about phasing out transrectal biopsies in the United States? https://chng.it/7bQsWSfK
Carpe prostata, as the ancient Romans might have said.
.



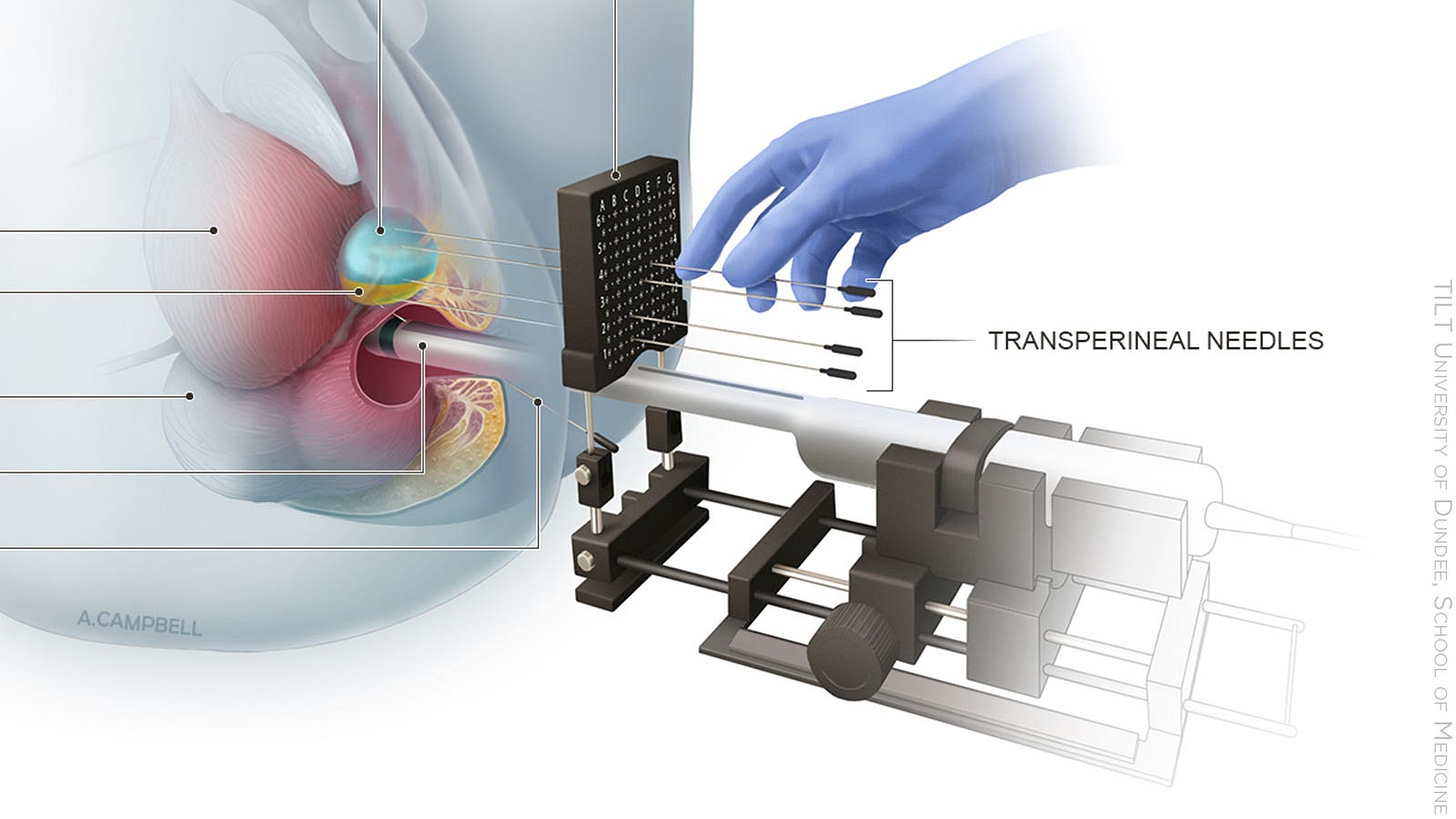
Many urologists have made the switch to transpeineal biopsies. That's in their interest and that of the patient.
Sepsis is dangerous.
But some urologists don't want to make any changes.
David Keller, an AS patient from Jax, told me:
"The chair of the urology department at [a brand-name hospital] in his own uses the transrectal method for prostate biopsies according to his PA 'because that’s how he was trained.'
"Just learned this last night from my friend who is being treated by this urologist, but this friend is taking advice from me to steer clear of the transrectal prostate biopsy."
Good work, David. Friends helping friends try to advise them against transrectal biopsies. Like Wilford Brimley said about oatmeal: It's the right thing to do. https://www.youtube.com/watch?v=D5LiwTVJrTk
Urologist Anthony Horan M.D. described many dangers waiting for those entering the prostate cancer arena. His book, "The Rise and Fall of the Prostate Cancer Scam" is an invaluable read for both patients and physicians.
The trans-rectal ultrasound-guided prostate biopsy is not only very risky but an embarrassingly unscientific test. This stupid test samples blindly and randomly about 0.1 percent of the prostate leaving you ignorant about what's going on in 99.9 percent of the prostate.
The trans-perineal biopsy scores better on risk but remains ridiculously unscientific. When the perineal biopsy is undertaken with a "fusion" imaging study, reliability is considered another advance. More accurate is an MRI-guided targeted biopsy of high Pirads areas by an expert in prostate imaging. Unbelievably irrational, the addition to this study of random biopsies sampling an extra 0.1 percent of the prostate is interpreted as being scientifically beneficial. Sadly, countless men continue to be in jeopardy of undergoing unnecessary, unreliable and debilitating testing and treatments for which there is no scientific evidence of life extension.