Prostate cancer passing breast cancer in some countries, while lagging in research/awareness
But the American Cancer Society that is not what's happening in the U.S.
By Howard Wolinsky
Prostate cancer is often said to be the male equivalent of female breast cancer. (Some men get breast cancer, too.)
But cases of breast cancer and deaths have outnumbered those of prostate cancer, and breast cancer has received the lionesses’ share of funding because of advocacy by women and their families adorned with pink ribbons.
Men generally neglect their own health for conditions like prostate cancer, heart disease, and everything else. It’s changing, but men and their advocates with blue ribbons also have not exerted political muscle in the male-dominated Halls of Congress, where some pols actually have had first-hand experience with prostate cancer.
U.S. Senator and former GOP Presidential Candidate the late Bob Dole made big news. Not so much for his prostatectomy. The news was mainly for the Kansas Senator appearing in ads that put those “little blue pills” on national TV that made Viagra dinner table conversation—and also ads for Pepsi featuring sexy Britney Spears with double entendres from the witty Dole.
Still, breast cancer has gotten more media attention and also research funding than prostate cancer. Easier to crusade for our wives, moms, and daughters for breast cancer than for our fathers, sons, and ourselves for the prostate gland, right?
But here’s today’s headline: In the near future, the incidence of and death rates from prostate cancer surpassing that of breast cancer.
Reston, Virginia-based Veterans Prostate Cancer Awareness makes this point in its campaign “Make Blue the New Pink,” referring to the ribbon colors for the respective cancers.
“‘Make Blue the New Pink’ was designed to bring attention to the reality that prostate cancer diagnoses are increasing, and nearing the number of breast cancer diagnoses.
“Just as pink ribbon awareness is synonymous with breast cancer, we hope to increase the recognition of blue ribbon awareness for prostate cancer as a similar symbol,” according to a news release from Veterans Prostate Cancer Awareness Inc., a non-profit organization focused on raising awareness and educating our nation’s veterans about the No. 1 diagnosed non-skin cancer within the Veterans Administration System.
There is some disagreement on this.
However, a spokesman for the American Cancer Society told The Active Surveillor that his organization is not predicting at this point that prostate cancer is surpassing breast cancer.
ACS chief scientific officer, Dr. William Dahut also said, “We do not expect a surge in metastatic disease. The number of patients presenting with more advanced disease has increased, however, with the change in USPTF (U.S. Preventive Services Task Force) Prostate Cancer PSA guidelines in 2018. We are hopeful that this trend will reverse.”
His message: “Fortunately, most men with prostate cancer will not die from the disease, and many will never know about their diagnosis. At this point, we do not anticipate prostate cancer cases surpassing breast cancer. If there was significantly greater number of prostate cancer biopsies performed in the US (biopsies done at lower PSA values) the incidence rate of prostate cancer would increase, but there is not evidence that this would decrease deaths.”
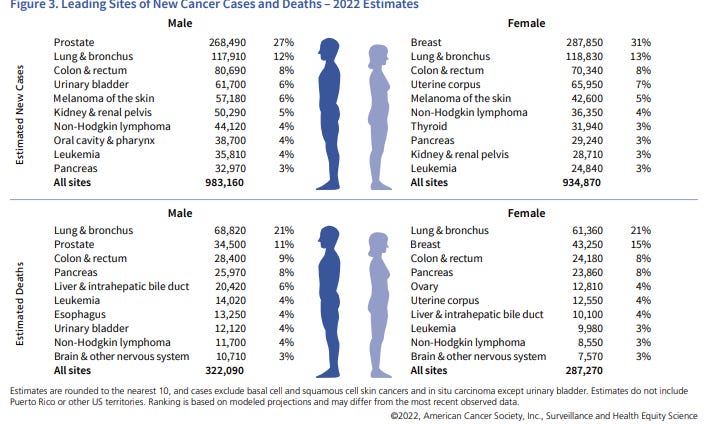
Veterans Prostate Cancer Awareness Inc. says in a few years, the line on the graph for prostate cancer will cross that for breast cancer. ACS contradicts this.
Almost 270,000 men will be diagnosed with prostate in 2022, according to the American Cancer Society. That’s 20,000 more than 2021. Plus there is an increase in the number of patients with advanced and metastatic prostate cancer as fewer men are undergoing PSA blood tests to try to detect cancer early. And many men shied away from medical attention during the ongoing COVID-19 pandemic, resulting in issues for those with prostate cancer.
Dahut said COVID likely will have an impact, but the numbers are not yet in. “It will likely have an effect, but we have to wait to determine the extent about a year for the availability of data from population-based cancer registries.”
The growth of prostate cancer is a global phenomenon:
—More men in the United Kingdom now die of prostate cancer than women die of breast cancer.
—Prostate cancer is the No. 1 killer of men in Sweden.
—The World Health Organization considers prostate cancer to be an epidemic in the Caribbean Basin.
—Breast cancer is no longer the most common cancer in Australia. Diagnoses of prostate cancer are forecast to surge by 34 percent, making it the most common cancer in the country.
—Prostate cancer in neighboring New Zealand is that country’s most diagnosed cancer.
Meanwhile, back in the USA, and elsewhere, research funding for prostate cancer lags that for breast cancer.
Funding is not based solely on the burden of disease but where top scientists think the biggest bang can be had for the buck—and it’s also influenced by the political clout that advocates and patients can muster.
Some examples of what may be seen as disparities: the U.S. National Cancer Institute research budget in 2020 was $515 million for breast cancer vs. $209 million for prostate cancer. The Congressionally Mandated Medical Research Programs spent $150 million for breast cancer and $110 million for prostate cancer in 2021.
Groups like ZERO are advocating for equitable funding. But that’s not easy because everyone thinks their pet cause ought to be on top.
Politics plays as big a role in the multibillion-dollar biomedical research enterprise as it does in defense contracts. The analogy is apt: Advocates for diseases “war” with one another for scarce federal dollars while researchers fight for the money.
Some conditions that need attention can be overlooked in the tussle because they are not sexy enough and their champions don’t have clout.
In 2019, researchers from Northwestern University in Chicago found things were even worse relating to private funding of research for prostate cancer vs. breast cancer.
“Breast cancer received the most funding by far, at $460 million, accounting for a third of all cancer-specific nonprofit revenue. Next in line—with less than half the funding of breast cancer—were leukemia ($201 million; 15% of total revenue), childhood cancers ($177 million; 13%), and lymphoma ($145 million; 11%). These cancers all received a greater share of funding relative to their proportion of total new cancer cases, mortality, and years of life lost.
“In contrast, colorectal cancer, pancreatic cancer, liver and bile duct cancers, brain cancer, lung cancer, prostate cancer, sarcoma, melanoma, and gynecologic cancers, including ovarian, cervical and endometrial cancers, were underfunded relative to the number of new cases, deaths and years of life lost.”
The researchers noted that cancers that are common but typically progress slowly or have a relatively low mortality rate, like breast cancer, have more survivors who can become advocates for the cause and attract more donors. Prostate cancer has a similar profile to breast cancer but it doesn’t have the clout of the breast cancer lobbyists.
A factor not mentioned by the researchers is the fact that breast cancer affects mostly women, so it receives attention and funding from organizations and political entities that support women’s issues—much as HIV/AIDS has received attention and funding from groups that support the LGBT community.
Where support comes in from private sources for prostate cancer, such as the Prostate Cancer Foundation, funding is largely earmarked for research on helping men with more advanced cancer. Men with low-risk to favorable intermediate-risk prostate lesions essentially are the Rodney Dangerfields of PCa—we get no respect.
“[Nonprofit organization] funding by cancer type is not proportionate with individual cancer burden on society,” the NU researchers concluded. “Disease stigma negatively impacts funding. A significant need exists to increase awareness and funding for many under-supported but common and highly lethal cancers.”
The researchers noted that underfunding may have negative repercussions for research, novel drug development, and the number of drugs approved by the Food and Drug Administration for poorly funded cancers.
How did women become so successful at raising funding for research funding?
Women, who are more health conscious, to begin with, became activists on behalf of breast cancer research.
As a reporter for the Chicago Sun-Times in the early 1990s, I was at ground zero for the breast cancer lobbying initiative. I was the lone reporter who covered a small, historic Chicago meeting where famed breast cancer surgeon and patient Dr. Susan Love made her call to arms for women to stand up for more research funding for breast cancer. She was taking a leaf from AIDS activists, who were able to win over policy-makers and health research funders to focus for the first time on patients with a stigmatized disease.
Breast cancer was on my map, in part, because my mother died from it. I wrote about prostate cancer occasionally, but I gave breast cancer more coverage. Sorry guys. I didn’t know then what I know now.
I was among the first reporters in the world to cover AIDS in the early 1980s—before it was called AIDS. (It originally was known as GRID—Gay-related Immunodeficiency.)
In the case of AIDS, savvy outsiders, not Congressional insiders, wrote the book on politicizing funding medical research. Fueled by rage, militancy, and newfound political prowess, advocates of greater funding for AIDS research achieved one of the great funding success stories ever.
I spent a year of my life writing only about AIDS/HIV early on in the epidemic.
Protesters successfully combined "die-ins" and other street theater with conventional lobbying to make splashes in Congress and the media on behalf of research on a disease that was killing ostracized gays and drug addicts. Advocates, driven by a health crisis in the gay community and a surge of political power as the community came out of the closet, were able to persuade Congress to devote funds to AIDS research.
Like the AIDS advocates, Love et al. seized the day and attracted many individuals to a successful campaign.
Is there a Susan Love for prostate cancer? Lots of famous men with the disease increased public awareness of prostate cancer, such as the late Generals Colin Powell and Norman Schwarzkopf, golfer Arnold Palmer and billionaire Warren Buffett.
(Note: Not many have spoken up for active surveillance. I can think of one: actor Bill Duke from Predator.)
In research, as in most endeavors, politics is often the tail that wags the dog.
It’s time for us all to stand up for prostate cancer in the public arena. Don’t be stigmatized by this common cancer. Ask your Congressional reps to support funding research. ZERO, for example, has been making progress with legislation to ensure insurance companies provide free access to prostate screening.
(I testified for the bill in Illinois. My old friend Gov. J.B. Pritzker recently signed it into law.)
Active surveillance has become a good news story as growing numbers of men sign up for it. But the overall story for advanced prostate cancer is worrisome.
It’s time for us to stand up for our brothers, sons, fathers, friends, and ourselves.
Meetings and more
Don’t miss: ASPI (Active Surveillance Patients International) will be premiering the first of a new video series titled “Active Surveillance 101" at noon Eastern on September 24, 2022.
Register here: https://bit.ly/3QGc8Uh
Like 101-level courses in colleges, AS 101 is aimed at teaching the basics. In this case, it's the basics of active surveillance, close monitoring of low- to favorable intermediate-risk prostate cancer.
The program features conversations between actual patients and their partners/spouses and leading experts. The goal of this series is to reach all AS candidates, including those who have not yet been diagnosed with prostate cancer but have rising PSAs (prostate-specific antigen) blood levels and offer them an introduction to AS and help them formulate questions when they go to their family doctors, urologists, or oncologists.
The first episode features a couple, Nancy and Larry White in a simulated office visit with Dr. Steve Spann, a top family physician and dean of the University of Houston College of Medicine. They discuss Larry's rising PSA and what it may mean.
The AS 101 series is aimed at patients who have not been diagnosed, the newly diagnosed and also patients who have been on AS for a while and want a “refresher course” on the basics. Partners and other loved ones will find it of interest.
In subsequent episodes, the couple visits Dr. Laurence Klotz, of the University of Toronto, the "father of active surveillance." Other episodes of AS 101 are being developed on biopsies, imaging, and DNA testing.
The AS 101 series is aimed at patients who have not been diagnosed, the newly diagnosed and also patients who have been ofnAS for a while and want a “refresher course.” Partners and other loved ones will find it of interest.
In subsequent episodes, the couple visits Dr. Laurence Klotz, of the University of Toronto, the "father of active surveillance." Other episodes of AS 101 are being developed on biopsies, imaging, and DNA testing.
AS 101 is sponsored by the Active Surveillance Coalition, which includes Active Surveillance Patients International, the AnCan Virtual Support Group for Active Surveillance, Prostate Cancer Support Canada, Prostate Cancer Research Institute, and TheActiveSurveillor.com newsletter. We encourage you to share this series with anyone you know who is dealing with this issue, including your family physician.
Sign my petition to phase out transrectal biopsies. Read why: https://chng.it/7bQsWSfK Once we hit 1,000 signatures, we should begin letting Congress, Medicare, and the American Urological Association know. Please make no donations. This effort requires your signatures, not your money—at this point.
Shout out to Dr. Jeremy Grummet, a leader in TREXIT (transrectal exit) movement:
If you’re on Twitter, you can follow me @journotwit.
More meetings for Prostate Cancer Awareness Month
The Walnut Foundation Monthly Meeting in support of Prostate Cancer Awareness Month.
Topic:-Incontinence, Erectile Dysfunction & Prostate Cancer with Special Guest. Dr. Emmanuel Abara, Urologist.
This is a free webinar. You may submit your questions in advance to info@thewalnutfoundation.com
Prostate Cancer Support Canada meets virtually. Yanks are welcome.
The Prostate Cancer Support Canada is holding its 2022 Prostate Cancer Virtual Conference September 17-18 in honor of Awareness Month.
Day 1, The ‘New Normal’ for Support Groups, will focus on facilitation and communication skills for those in, or interested in, leadership roles in the prostate cancer support community.
Day 2, Prostate Cancer Realities will more broadly address issues of interest to our community including managing anxiety and stress throughout the cancer journey, genetics and prostate cancer, upcoming research, how to find trusted information about prostate cancer, and more.
Dr. Brian Goldman, best-selling author and host of White Coat, Black Art on CBC radio, will be speaking about The ‘New Normal’ for Support Groups.
Check for details in the conference program ‘flipbook’ with session + speaker details and registration link: https://bit.ly/2022PCVCprogram
Prostate Cancer Foundation is looking at physical and mental illness.
For Prostate Cancer Awareness Month, the Prostate Cancer Foundation, the 800-pound private prostate cancer researcher, is holding a webinar on “Physical and Mental Wellness in Prostate Cancer.”
Here are the details:
Join us for the first in a series of monthly webinars hosted by PCF President and CEO Dr. Charles J. Ryan.
During Prostate Cancer Awareness Month, PCF challenges everyone to Get Healthy. Dr. Ryan and guests will discuss key aspects of nutrition, exercise, and mental health in prostate cancer.
The event will be Sept. 20, 2022 04:30 PM in Pacific Time (US and Canada).
Sign up to join here.
Following each segment, there will be a live Q&A.
• Prostate 8: Simple lifestyle changes that work (Dr. Stacey Kenfield, UCSF)
Dr. Kenfield is an Associate Professor in the Department of Urology and is the Helen Diller Family Professor of Population Science for Urologic Cancer. She is an expert on lifestyle, exercise, nutrition, and their impact on prostate cancer. She'll discuss research showing how specific lifestyle factors improve outcomes after prostate cancer diagnosis, and practical ways to incorporate these changes into your life.
• Mental Health and Prostate Cancer (Dr. Andrew Roth, Memorial Sloan Kettering Cancer Center).
Dr. Roth is an Attending Psychiatrist and is board-certified in Psychiatry, Geriatric Psychiatry, and Psychosomatic Medicine. He is focused on caring for the mental health needs of patients with prostate cancer and other genitourinary diseases. He'll provide an overview of the challenges patients commonly face, as well as strategies and resources for coping and living well during treatment and survivorship.
Here’s hoping Dr. Roth will cover AS as well as advanced prostate cancer.
Please send any questions for the speakers in advance to: webinar@pcf.org







Well put! Just as disturbing to me is the the lack of attention by oncologist and urologists to the emotional wellness of women and men that are diagnosed with breast and prostate cancer. Richard
Thanks for mentioning those issues, Richard.